We’ve all sat in our homes and waited with bated breath, and checked the clock every few minutes for what felt like an eternity for test results. After having a scan or blood work done, we then sit for days, hoping for the best. Wouldn’t it be wonderful if we could reduce the time we have to wait for test results and improve their accuracy?
Hospitals across the U.S. are implementing new technologies to both reduce the time it takes to get test results and improve accuracy. But let’s be honest, these “tools” won’t be the movie “Robot Doctor.” These tools will probably be more along the lines of a persistent, smart assistant to help doctors whom we have grown to trust.
Consider how overwhelming it would be for your doctor to develop the very best course of action to treat you for whatever health issue(s) you have, while simultaneously managing hundreds of patient charts, endless lab tests, and research studies in their area of expertise.
Processing such massive amounts of data would be difficult enough for even a computer program. Artificial intelligence in medicine was developed to act as a high-powered filter that can sift through an enormous volume of data almost instantly, and assist doctors in identifying trends or patterns in that data that they might otherwise overlook. With AI assisting the doctors, they would be able to concentrate on what truly matters – YOU.
Today, many U.S. hospitals are employing AI to assist radiologists in reading mammograms and CT scans. The primary role of AI in reviewing mammograms or CT scans is to serve as a secondary pair of “expert” eyes, helping the radiologist detect smaller potential issues they may have overlooked due to fatigue from extended work. The use of AI has been documented in the industry in several ways, most notably by streamlining hospital logistics through automated appointment scheduling, which ultimately reduces wait times.
All applications discussed above are based on the same premise: using smart software to enhance the speed, safety, and effectiveness of healthcare delivery.
In addition to improving patient appointment scheduling, AI is used in Healthcare in the USA in numerous ways to help doctors make diagnoses more effectively. Furthermore, AI will serve as the foundation for developing customized treatment plans for patients based on their unique medical needs, providing the most personalized healthcare delivery ever.
#Complete Guide: Success & Powerful Best AI Tools for Business in USA
Summary
The purpose of this guide is to show all the ways AI is revolutionizing healthcare throughout America — and will continue to do so — as a quick, data-based doctor’s assistant in creating better, faster, and more individualized care. In addition to describing the many positive changes it creates, the guide begins by showing the negative experiences most patients go through during their medical visits — waiting too long for test results or for scheduled appointments to be made and received.
With AI technology, long waits are being eliminated as it quickly reduces wait times and greatly increases the accuracy of test results — especially when there is a large amount of information to review.
Following up on the previous example, the guide goes on to describe other ways AI is helping to create higher-quality care. First, AI technology is being used in hospitals to help with administrative and scheduling tasks. By using AI, hospital administrators can find available time slots for future appointments sooner than before, send reminder notifications to both patients and staff about upcoming appointments, and reduce the paperwork required for each visit.
Secondly, AI enables the creation of tools that allow clinics to electronically record and summarize clinicians’ notes from previous patient visits. This gives clinic professionals (i.e., Doctors and Nurses) more time to focus on providing higher-quality care to their patients, rather than spending unnecessary hours on recording and documenting their care.
AI’s role in providing personalized therapies is growing rapidly, according to the guide, by using Big Data to compare individual patient data with large-scale databases of clinical outcomes, enabling clinicians to determine and use the most likely successful treatment from those available and avoid the trial-and-error approach.
In addition to the above, the guide covers the advent of patient-facing products such as wearable devices and health apps that provide a basis for establishing a baseline of what is normal for each person and alerting both the patient and their healthcare provider to possible dangers.
Lastly, the guide also includes a review of AI in drug development and robotic-assisted surgery. In robotic-assisted surgery, the physician maintains complete control throughout the surgical procedure but uses technology to improve the precision and accuracy of their actions.
In summary, the guide stresses the need to protect confidentiality (HIPAA) and to avoid biases in AI decision-making. The overall message or theme of the guide is that AI is utilized at its best when it assists the clinician, enhances their expertise, and places the patient at the center of their medical care.
AI is used in healthcare in the USA: AI is used in healthcare in the USA to improve patient care, enhance diagnostics, and streamline hospital operations

The application of AI is used in Healthcare in the USA provides numerous benefits to enhance the quality of healthcare delivery. AI can help clinical staff recognize early warning signs and other patient health issues, enabling them to choose the best course of action based on the AI’s recommendations. This will result in faster and better care for each patient. The additional benefit of using AI in this capacity is that it may help reduce treatment delays caused by inefficiencies in clinical decision-making.
In addition to its use as an aid in clinical decision-making, AI is used in Healthcare in the USA to support nurses and physicians in their daily clinical workflow. AI can generate reminders, summaries, and checklists to help prevent errors and omissions in patient care. Another function of AI in supporting clinical decisions is matching a patient with the appropriate level of care (e.g., telemedicine visit, urgent care, emergency department), enabling the patient to receive needed services as quickly as possible while minimizing unnecessary crowding in emergency departments.
Another area of AI is used in Healthcare in the USA is improving the speed and accuracy of diagnostic processes; specifically, AI can improve diagnostic processes associated with imaging studies and laboratory tests. In radiology, AI can generate flags that identify areas of concern (e.g., stroke, lung nodules, fractures, breast cancer) on imaging studies, enabling faster evaluation by clinicians. This process enables clinicians to prioritize more serious cases when determining which patients require immediate medical care.
In the AI is used in Healthcare in the USA is enhancing the capacity of health care providers to assess and monitor patients in a variety of settings (e.g. within hospitals and outside hospitals).
Wearable devices and remote patient monitoring technologies enable providers to collect data on physiological parameters (e.g., heart rate, oxygen saturation, blood glucose levels) and alert them when changes indicate potential problems that should be addressed. Additionally, AI is being used to identify patients who will require greater assistance with chronic diseases and to alert them to potential complications, so they can be contacted and appropriate measures taken to prevent them.
Using predictive models and analytics in hospitals, warning signs of impending sepsis, falls or readmissions are identified early enough for caregivers to intervene to avoid emergency situations.
In addition, AI is used in Healthcare in the USA to support hospital operations by automating workflows. Using scheduling applications, AI helps eliminate unused appointment times and ensures the appropriate number of personnel are available during the correct time frame.
Many routine administrative activities (e.g., documenting visits, summarizing charts, securing prior authorization) are handled by AI is used in Healthcare in the USA, enabling clinicians to spend additional time with their patients. Supply chain management applications use AI to forecast demand for medications and supplies; bed management applications support admissions, transfers, and discharges.
Although AI can offer many advantages to how a hospital runs, there are some considerations when AI is used healthcare in the USA. If the models created by AI do not use a balanced representation of the entire community in the training data used to develop them, they may “reflect” these imbalances and thus increase existing disparities. Privacy and Security concerns arise with the use of AI in healthcare because of the HIPPA restrictions placed upon healthcare data in the U.S.A.
When AI is used in healthcare in the USA., there should be established local governance processes (audit trails, etc.) so that the organization has control over how models work in their environment and perform locally.
Overall, AI is used in healthcare in the USA to assist with improving diagnosis, supporting patients’ needs, and assisting in making hospitals run more effectively; however, for AI to reach its full capabilities, it will need to be used as “teamwork technology”, not as an alternative to clinicians’ input. Programs that utilize successful AI will rely on sound data management practices, transparency in evaluations, and open communication about how recommendations were developed.
Artificial Intelligence Medicine in the USA: Discover how artificial intelligence medicine is transforming diagnosis, treatment, and clinical decision-making in the USA.

AI medicine in the USA has evolved beyond pilot trials to become a standard component of care; it will alter how clinicians diagnose disease, choose treatment, and ultimately make their decisions when providing care. The strength of AI medicine in the U.S.A. lies in its ability to supplement an experienced clinician’s decision-making by leveraging image- and lab-based data and historical pattern recognition. Many health systems in the USA have transitioned from pilot projects to a common clinical tool, altering how clinicians find diseases, select treatment options, and make clinical decisions at the point of care.
The power of Artificial Intelligence Medicine in the USA lies in augmenting an expert clinician’s judgement using pattern recognition across images, laboratory data, and patient medical history. In many health systems, AI is used in healthcare in the USA to shorten wait times, highlight previously undetected risk factors, and provide standardized best-practice recommendations, particularly in areas with high volume and time/attention constraints.
Artificial Intelligence Medicine in the USA is changing Radiology and Emergency Triage. Algorithms can identify potential strokes on CT scans, indicate probable causes of lung abnormalities, and/or place suspicious mammogram exams at the top of the list so they are seen first by radiologists.
Artificial Intelligence Medicine in the USA to assist clinicians in finding subtle patterns that may be missed during periods of high activity, while still allowing licensed professionals to interpret the findings. In Pathology, AI Medicine in the United States assists pathologists with slide review by highlighting regions of interest and quantifying tumor characteristics related to subtype and prognosis, thereby creating greater consistency among pathologists.
Treatment is also undergoing changes, as Artificial Intelligence Medicine in the USA is being integrated into Precision Medicine Programs.
AI models can integrate genomic information, prior treatments, imaging studies, and outcomes to recommend treatment options to tumor boards and identify patients who could benefit from clinical trial participation. for purposes of shortening waiting times, identifying new or previously unidentified risk factors and making standardized recommendations based upon established best practices, most notably where there are both high volumes and limited time/attention.
The future of Radiology and Emergency Triage is being transformed by AI medicine in the U.S.A. For example, algorithms can identify possible stroke signs on CT scans, probable causes of lung abnormalities, and prioritize suspect mammograms for radiologists to review before others.
While reducing variability in what a clinician sees, AI medicine in the U.S.A. is enabling clinicians to discover subtle patterns that may be missed during periods of high productivity and to continue interpreting results. In addition, AI medicine in the U.S.A. is assisting pathologists in the review of slides by highlighting specific regions of interest (e.g., tumors) and quantifying tumor characteristics which relate to the type of cancer (subtype), stage of cancer (prognosis). These features will enable pathologists to provide consistent interpretations regarding cancers.
In terms of Treatment, AI medicine in the U.S.A. is beginning to transform how clinicians make treatment recommendations within Precision Medicine Programs. Specifically, AI models can integrate genomic data, prior treatments, imaging data, and outcomes to provide tumor boards with evidence-based recommendations and to determine which patients are eligible for enrollment in clinical trials.
AI is used in Healthcare in the USA to optimize prescription options; therefore, it assists with calculating proper medication dosages and forecasting potential side effects or dangerous drug-drug interactions for complex patients.
Artificial Intelligence Medicine in the USA also has applications in surgical planning and radiation oncology. It supports in the areas of anatomical mapping, margin estimation, and automated contouring processes so that clinicians are able to make high-value clinical decisions.
Regardless of specialty, clinical decision-making could possibly become one of the main use cases for Artificial Intelligence Medicine in the USA. Examples of these decision-support tools include estimated risk of developing sepsis, likelihood of returning to the hospital after discharge, and the best available evidence-based pathway for each patient based on their individualized needs.
AI is used in Healthcare in the USA to analyze large volumes of medical information in patients’ medical charts, generate patient visit note templates, and organize patients’ problem list data. Therefore, AI-Assist can help alleviate some of the documentation-related burdens placed on providers, allowing them to allocate additional time to direct patient care.
In addition to improving the delivery of health care through the use of artificial intelligence (AI) technology in the U.S. physical examination room, AI is also being utilized to enhance the operation of health care systems and thus influence patient experience. AI-driven scheduling models help minimize missed appointments and align staff schedules with demand. Capacity management uses AI to support bed management, transfer management, and discharge planning.
Revenue cycle activity is also supported by AI is used in Healthcare in the USA Coding and documentation related to prior authorization are examples of this type of activity, which ultimately reduces the amount of time it takes for administrative delays to resolve claims prior to providing treatment.
Patient safety and trust are of paramount importance. Testing for bias and validating all AI systems used in medicine in the U.S. must occur in real-world clinical settings. Once an AI system is implemented, it will need to be continuously monitored for issues related to data drift, workflow changes, or other factors that may impact the ability of an AI system to continue recommending accurate solutions over time.
As AI is used in healthcare in the USA, regulatory requirements and standards for maintaining the confidentiality and security of patient-identifiable information will be required for many types of AI applications.
Many AI-based health care applications will require providers to maintain records of when they choose to rely on AI recommendations and when they override them. Strong governance and transparency practices, combined with sufficient education/training for providers who use these tools, provide a framework for responsible expansion of AI in medicine in the U.S.
#Complete Guide: Leading & Innovative Best Robotics Companies in USA
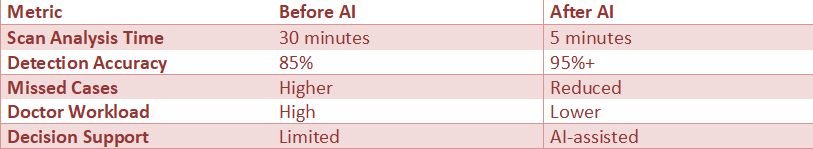
AI vs Traditional Healthcare
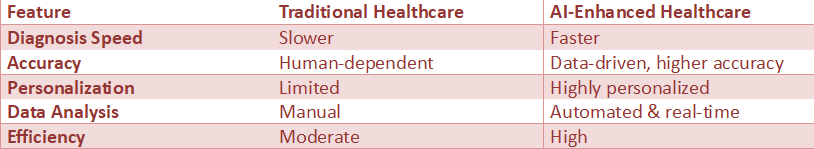
Insight: AI enhances, not replaces, doctors by improving speed, accuracy, and personalization.
Source:
- IBM Watson Health
https://www.ibm.com - McKinsey Healthcare AI Report
https://www.mckinsey.com
Healthcare AI applications in the USA: Explore real-world healthcare AI applications improving hospital efficiency and patient outcomes

AI is used in healthcare in the USA; it is no longer experimental, it’s now being used to enhance efficiency and care quality by hospitals, clinics, and healthcare systems. Many in the U.S. have found ways to use AI in the healthcare system in the U.S. To eliminate delays and avoid unnecessary harm, so that providers may be able to focus on providing patient care instead of doing paperwork.
The most successful Healthcare AI applications in the USA will include high-quality data, defined workflows, and human oversight, so that AI does not replace provider decisions but assists providers in making them.
The majority of Healthcare AI applications in the USA Fall under the category of “operational command center” support. Operational command center support includes AI is used in healthcare in the USA system to forecast patient volume, anticipate bottlenecks, and create more accurate and efficient staffing models based on units and shifts. These tools allow hospitals to avoid last-minute scrambles, minimize overtime, and maintain smooth operations in critical areas—including the Emergency Department.
Another type of Healthcare AI application in the USA is scheduling optimization, which uses patterns from cancellations and no-shows to identify gaps and close them to reduce wait times.
In addition to reducing operational stressors within a hospital setting, Healthcare AI applications in the u.s. Also are also used to improve patient flow. Some systems use data analysis to determine whether a patient is ready for discharge and whether any barriers to discharge exist (e.g., pending lab results, delayed consults, need for transportation).
This allows the clinical staff to take action before the patient is discharged and, therefore, make a bed available to an incoming patient.
AI is used in healthcare in the USA system to optimize admissions, transfers, and discharges. As a result, the number of hand-offs required across departments has been reduced, and time spent communicating across departments has decreased.
Although the use of Healthcare AI applications within the United States results in positive clinical outcomes when applied early to inform clinical staff regarding a patient’s clinical status, there are also numerous U.S. hospitals utilizing early warning models to alert staff to the potential for a patient to experience sepsis, respiratory decline or an unplanned admission to the ICU.
AI offers an opportunity for a clinician’s inquiry into a patient’s clinical status to prompt a timely laboratory test or examination, if properly implemented, thereby allowing the clinician to act before the patient becomes clinically unstable. Of key importance is that alerts from Healthcare AI applications need to be “fine-tuned” so they do not contribute to alarm fatigue and align with Registered Nurses’ workflow.
The deployment of Healthcare AI applications throughout the United States has transitioned from experimental to implementation-based, on the belief that the successful application of AI in healthcare will improve operational efficiency and enhance the quality of care.
Many organizations in the USA use AI in healthcare to eliminate delays, prevent unnecessary patient harm, and allow clinicians to spend more time caring for their patients and less time on administrative tasks. Successful Healthcare AI applications in the United States will rely on high-quality data, well-established workflows, and human oversight to ensure that AI supports, rather than replaces, clinician decision-making.
Approximately one-half of Healthcare AI applications in the United States fall under the category of operational “command center” support. This includes AI is used in healthcare in the USA to forecast patient volume, recognize potential bottlenecks, and generate more precise and effective staffing schedules by unit and shift. Such tools can help hospitals avoid last-minute scrambles, reduce overtime, and maintain steady operations in critical departments, including the Emergency Department.
The other half of Healthcare AI applications in the United States apply scheduling optimization techniques. These technologies analyze trends in cancellations and no-shows, allowing them to identify and fill gaps while shortening wait times.
Inpatient settings are the primary locations where Hospital Healthcare AI applications in the USA are applied to address patient throughput issues. Examples include analyzing a patient’s status to determine whether they are ready for discharge and identifying potential barriers to discharge (e.g., pending labs, delayed consultant, need for transportation). With this AI application, the clinical team can address identified barriers to discharge before the patient’s actual discharge date, thereby making beds available for other patients.
AI is used in Healthcare in the USA, and is being utilized in order to optimize admissions, transfers, and discharges within hospitals, thus reducing the number of times patients have to be handed off from one department to another, as well as the time it takes for interdepartmental communication.
The implementation of Healthcare AI applications in the USA results in improved patient outcomes when clinical staff receive information regarding their patient’s clinical status sooner rather than later. Several hospitals are utilizing early warning models to alert clinical staff to a patient’s potential clinical deterioration, such as sepsis, respiratory decline, or an unplanned ICU admission.
AI may prompt a timely check or lab test in response to a clinician’s inquiry about a patient’s clinical status, enabling the clinician to intervene if the patient becomes clinically unstable. However, it should be noted that AI-generated alerts require “tuning” to prevent alarm fatigue and to mimic registered nurse workflow.
Impact of AI in Healthcare
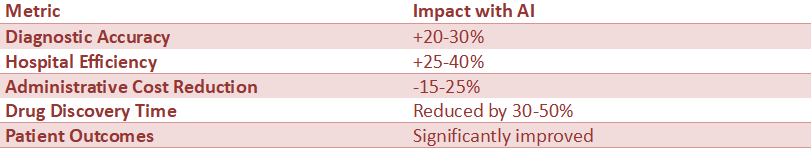
Key Insight: AI is improving both clinical outcomes and operational efficiency.
Source:
- Deloitte Healthcare AI
https://www2.deloitte.com - Statista Healthcare AI
https://www.statista.com
AI healthcare solutions in the USA: Learn about innovative AI healthcare solutions reshaping modern medical systems

AI Healthcare Solutions in the US Are Helping Providers Make Better Decisions by Leveraging Large Volumes of Clinical and Operational Data to Improve Response Timeliness.
The most practical AI Healthcare Solutions in the US focus on solving everyday problems for providers. These include delays, missed early warnings of risk, and the time providers spend documenting and processing information.
One important group of AI Healthcare Solutions in the US has the ability to detect risks sooner with vital sign trend analysis, lab trend analysis, and analyzing a patient’s history to notify their caregiver(s) when there could be a risk for developing serious medical emergencies like sepsis, respiratory failure, or readmission.
Using AI healthcare solutions in the US enables caregivers to be notified at the right time, so they can take action before a situation turns into an emergency. Used appropriately, these tools will provide both transparency and evidence-based validation of alerts while also helping to prevent “alarm fatigue.”
Another area where AI healthcare solutions in the US are growing quickly is in diagnostic applications. In Radiology, AI healthcare solutions help providers by prioritizing CT scans that show possible acute conditions (such as stroke, pulmonary embolism, or internal bleeding). In Pathology, AI healthcare solutions detect and quantify abnormalities in images of patients’ tissue samples and then assist in measuring them.
AI Healthcare Solutions in the US Are Helping Providers Make Better Decisions by Leveraging Large Volumes of Clinical and Operational Data to Improve Response Timeliness.
The most practical AI Healthcare Solutions in the US focus on solving everyday problems for providers. These include delays, missed early warnings of risk, and the time providers spend documenting and processing information.
One important group of AI Healthcare Solutions in the US has the ability to detect risks sooner with vital sign trend analysis, lab trend analysis, and analyzing a patient’s history to notify their caregiver(s) when there could be a risk for developing serious medical emergencies like sepsis, respiratory failure, or readmission.
Using AI healthcare solutions in the US enables caregivers to be notified at the right time, so they can take action before a situation turns into an emergency. Used appropriately, these tools will provide both transparency and evidence-based validation of alerts while also helping to prevent “alarm fatigue.”
Another area where AI healthcare solutions in the US are growing quickly is in diagnostic applications. In Radiology, AI healthcare solutions help providers by prioritizing CT scans that show possible acute conditions (such as stroke, pulmonary embolism, or internal bleeding). In Pathology, AI healthcare solutions detect and quantify abnormalities in images of patients’ tissue samples.
Healthcare clinics and hospital organizations in the U.S. have begun to utilize artificial intelligence (AI) in many areas of their operations and patient access; specifically, AI has been used to schedule appointments and to manage bed capacity. Predictive modeling can be used by scheduling application software to assess which patients are likely to miss their appointments (“no shows”), thereby allowing the health care organization to adjust its schedules.
Additionally, capacity management models may be used by a health care organization to assist in determining the location of an incoming patient when a bed becomes available, as well as assist in developing discharge plans.
The primary benefit of utilizing AI in these capacities is to reduce wait times for both patients and staff, increase the number of patients treated within a clinic during a specific period, and better manage staffing levels. In addition, some organizations have developed AI-enabled solutions to support call-center triaging and digital front-door initiatives. These AI solutions enable patients to determine the best course of action to receive appropriate care at the least cost and ultimately create a positive experience.
Whether or not AI solutions for healthcare will prove successful in the United States depends on several factors, including trust and governance. Healthcare organizations must develop robust policies to protect the confidentiality of patients’ medical information, ensure security measures are in place across all systems, and regularly evaluate each deployed model for potential biases. If a healthcare organization develops these necessary safeguards, it can implement AI-based solutions that improve safety, efficiency, and equity across various healthcare delivery settings.
Machine learning healthcare in the USA: See how machine learning in healthcare enables predictive analytics and personalized care

Traditional Methods: Limitations of traditional approaches include the inability to predict future risk based on pre-established rules. A key limitation of traditional approaches is their reliance on established rules. Machine learning enables clinicians to identify new patterns in EHRs, imaging studies, lab results, claims, and other data. This new method of pattern recognition can help clinicians identify patients at high risk of deterioration before an emergency develops.
In addition to applying machine learning in healthcare in the USA for Risk Stratification and identification of patient populations at high risk for complications (e.g., readmissions), hospitals also use machine learning models to predict the risk of sepsis, unplanned ICU transfers, falls, etc.
The purpose of using AI is used in Healthcare in the USA, the primary reason for this application is to enable clinical teams to prioritize attention towards patients most likely to deteriorate and develop complications; order tests sooner rather than later; and intervene earlier than would be possible without the assistance of AI is used in healthcare in the USA.
As previously stated, both imaging and digital pathology benefit from the application of machine learning in healthcare in the USA. When radiologists use algorithms, they can determine which studies may reveal acute stroke, internal bleeding, pulmonary embolisms, etc., thereby reducing the time required to review studies in urgent cases.
Additionally, when pathologists use models, they highlight suspicious regions on slides and standardize measurements linked to prognosis. AI is used in healthcare in the USA to improve consistency, while licensed clinicians remain responsible for final interpretation and patient communication.
A final area where machine learning is being applied in healthcare in the U.S. is in personalized care. By combining data points such as medical history, social factors, past outcome(s), and current signals, models can suggest tailored outreach plans, education needs, or pathways for future care. For instance, machine learning can be used in chronic disease programs to identify those heart failure patients trending toward decompensation and diabetics who are at a greater risk of complications.
AI is used in healthcare in the USA for personalization, allowing health systems to focus their resources on patients who would benefit most from this technology and improve outcomes without overloading staff.
Machine learning in healthcare in the USA. is also an example of how it has enabled individualized approaches to addressing patients’ needs through practical applications that benefit all patients. This is achieved through the use of machine learning to predict potential adverse drug reactions (adverse drug events) and identify potentially dangerous drug-drug interactions that could place patients at risk. Machine learning may also suggest patient monitoring requirements for patients prescribed multiple medications or with one or more complex chronic diseases.
Artificial intelligence (AI) used in pharmacy and inpatient settings will improve the quality of care by reducing preventable harm, increasing the timeliness of clinical issue detection, and offering clinicians alternative, safe therapeutic choices. Additionally, machine learning will help improve medication compliance by identifying patients most likely to miss scheduled refill appointments and initiating timely interventions to address them.
Machine Learning in Healthcare in the United States enhances operational processes in healthcare delivery by increasing accessibility and efficiency, leading to noticeable improvements in patient experience (e.g., reduced wait times, easier hospital discharge processes, better service coordination).
Machine learning healthcare in the United States utilizes scheduling algorithms to decrease “no show” rates and enhance template-based appointments. Additionally, capacity models can predict bed demand and identify patients who may pose a barrier to their discharge.
By utilizing machine learning in healthcare in the United States, it creates streamlined workflow processes so that clinicians have the ability to focus on providing direct care rather than on administrative processes. However, machine learning in healthcare in the United States must be appropriately monitored and maintained to prevent the need to validate models for local populations, monitoring model “drift,” and reviewing for potential bias and privacy issues.
Machine learning in healthcare in the United States is used to provide predictive analytics and personalized care by converting large volumes of complex data into timely, actionable information. The greatest benefits from the widespread adoption of AI in healthcare in the United States will be realized when high-quality models are integrated with clearly defined clinical pathways, human oversight, and continuous evaluation and validation to ensure that the technology used does not adversely affect the quality or equity of care delivered to patients.
AI patient care in the USA: Understand how AI patient care tools enhance monitoring, support, and treatment accuracy.

AI patient care in the USA will no longer be limited to automated systems. Rather than relying solely on an automated system for AI-driven patient care in the USA, we will have a complete set of operational tools. These tools will help the clinician observe his/her patients more closely, respond promptly, and make the best possible treatment decisions for each patient.
Currently, AI, in the form of analyzing large amounts of data for each patient (e.g., vital signs, lab test results, images, documentation, and history), is being used in hospitals and clinics to provide clear indications of what should happen next in patient care. To work well, AI-driven patient care in the USA must support clinical teams. This means it must reduce the frequency at which important pieces of information are missed and shorten the time for safe decision-making by clinical teams.
While there are numerous ways that AI patient care in the USA, possibly the most significant area impacted has been the ongoing monitoring of patients while they are hospitalized. While continuously tracking all the “streaming” vitals, lab tests, and documentation provided by nurses regarding a patient, an AI system may detect early warning signs of a patient’s decline from baseline status (such as impending sepsis or respiratory failure).
A second area in which AI patient care in the USA has made significant contributions to medicine is remote monitoring of patients with chronic diseases. This may be done using wearable devices or home-based monitors that allow doctors to continuously collect data on patient information such as blood pressure, glucose levels, oxygen saturation, body weight, and reported symptoms.
Through a machine learning model, concerning trends (e.g., fluid accumulation in congestive heart failure) can be identified and communicated to the physician’s office well before the patient experiences severe illness. Early contact, subsequent medication adjustment(s), and/or scheduling a same-day appointment will also help prevent unnecessary emergency department visits. AI patient care in the USA allows many patients to create care plans around their lifestyle routines instead of coordinating their lives around in-person appointments at a physician’s office.
When used to support clinical decision-making, AI patient care in the USA will continue to be an important tool for providing quality medical treatment to patients. Clinical decision support systems are available and will enable AI to present evidence-based pathways, identify contraindications, and assess the risk of complications (e.g., those related to patient-specific characteristics), thus supporting AI patient care in the USA for patients with numerous health issues and little margin for error.
AI is helping create safer patient experiences by rapidly and consistently escalating results from various diagnostic processes, including imaging and laboratory tests; it will also help ensure timely treatment for a variety of conditions. Studies have demonstrated that AI can both shorten timeframes and make diagnostic support (and consequently the quality) more reliable by decreasing the number of potential ordering or processing errors with regard to diagnostic testing.
AI is enabling several additional innovative applications beyond enhanced diagnostic support and communication in the area of AI patient care in the USA Examples of these innovations include: chat-based symptom triage; post-visit education; and follow-up reminders to provide patients information about what they may experience during their recovery period, when to call the clinician if there are concerns, and how to take medications as directed.
Educational materials created via AI patient care in the USA are frequently tailored to each individual’s reading level and/or preferred language, which can lead to greater adherence to planned treatment programs and less confusion for patients following an office visit.
To provide the American people with trust in using AI patient care in the USA, it must first be shown that AI is used in healthcare in the USA, a) safe and b) fair. Thus, the tools must be tested in actual clinical settings; their function must be continually monitored to identify changes in performance; and their effectiveness across different patient groups must be confirmed to account for potential biases.
In addition, clinicians must have direct pathways to review and escalate all decisions made in conjunction with AI. AI is designed to assist the clinician’s decision-making process rather than to make the decisions alone. In order to maintain patient confidentiality and protect sensitive information collected from patients at home or through patient messaging systems when using AI for patient care in the USA.
Ultimately, the use of AI in patient care in the USA has the potential to increase treatment accuracy and the timeliness of interventions, and to improve the overall quality of care by allowing clinical teams to respond faster and more reliably. However, the benefits of AI is used in healthcare in the USA will be determined by the quality of the information upon which the AI system was built and how carefully the design of the workflow considered how technology could positively affect care without creating unnecessary complexity.
#Complete Guide: Leading & Revolutionary Top Quantum Computing Companies in USA
Tired of Waiting? How AI Is Fixing Hospital Scheduling and Paperwork
It seems to affect almost everyone at some point. Frustration with calling and getting through to a doctor’s office and finding that a specialty physician is unavailable for weeks – if not months — following the initial phone call. Finding a doctor has become a massive issue – prior to meeting your doctor, you will likely need to successfully maneuver a complex scheduling maze.
One of the primary (and most tangible) ways Artificial Intelligence is being utilized in health care in the United States; rather than having a receptionist manually check the availability of just one doctor, AI is capable of quickly reviewing the availability of all physicians who are qualified within a given hospital system, looking for open time slots based on canceled appointments and providing you with the earliest possible time slot.
AI-based “smart” systems will also be able to automatically send appointment reminder messages, complete electronic pre-appointment paperwork, and send follow-up instructions via e-mail or text messaging. Overall, this should serve as a highly efficient assistant that works for both you and the hospital.
By allowing patients to receive care sooner and reducing wait times by increasing the speed at which they can access medical treatment, hospitals can better manage their resources. This results in less frustrated patients awaiting care due to a large backlog.
While there is growing interest in using artificial intelligence (AI) to assist in delivering healthcare services across the United States, one major area where AI can have a significant impact is reducing administrative burdens on physicians. In order for your physician to concentrate on you and not a computer screen, there are numerous administrative tasks currently being performed by your physician that could be significantly reduced with AI technology.
For example, using voice-to-text software, AI can generate a permanent record directly from your physician’s speech and summarize large amounts of lab test data in an easily understandable format.
This reduction in the administrative responsibilities for physicians and nurses will enable them to spend additional time with patients and create a more personal experience. The increased efficiency created by the development and implementation of AI technologies across healthcare will lead to two positive outcomes: faster access to medical services and increased physician availability at the times when patients need them most. In addition to assisting with data organization, AI will help physicians interpret and understand this data.
Giving Doctors a Second Pair of Eyes: How AI Helps Read Your Scans
There have been major advancements in how medical professionals interpret medical images. When an X-ray, MRI, or CT scan is completed, a patient waits for their test results to be reviewed by a specialist, a radiologist. While the patient waits, the radiologist examines the test results, looking for symptoms of disease. Artificial Intelligence (AI) works like an intelligent, highly knowledgeable assistant, helping radiologists review millions of test results to prevent missing anything.
How does it work? There is a large library of anonymized medical images with clearly defined diagnoses (e.g., thousands of mammography images with and without evidence of cancer). As the AI reviews this multitude of examples, it learns to recognize the subtle details that exist among all diseases. For example, the AI could find a small nodule in the lungs or detect a faint shadow in a lung image that even a trained eye might miss, especially if the doctor had been working long hours and was tired.
In essence, the AI acts as a safety net for diagnostic error. Diagnostic errors are reduced when the AI identifies potential trouble spots for the doctor to review. By consistently identifying abnormalities, this technology enables physicians to quickly diagnose and develop better treatments for their patients. In hospitals across the United States that use machine learning technology for medical diagnosis, doctors report increased confidence in their decision-making and in prioritizing the most critically ill patients.
One important aspect of AI is that it never makes a final decision. The AI identifies specific areas of interest in scans that require further evaluation by a human radiologist. Ultimately, the doctor will use both their years of training/medical education and the information provided by the AI to determine the final outcome of the test. The physician will always retain control over your medical care.
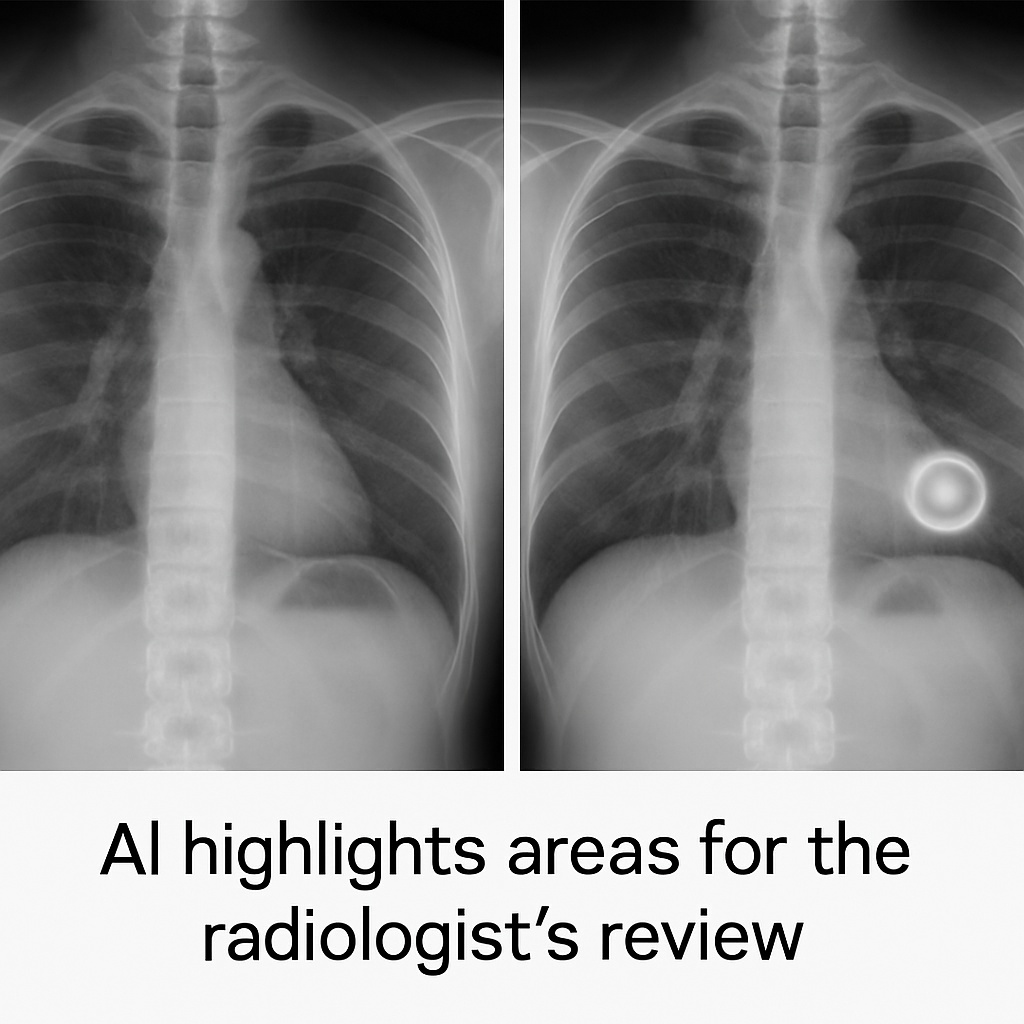
AI highlights areas for the radiologist’s review.
Real-World AI Diagnosis Example
Example: AI can detect early-stage cancer in scans faster and more accurately than manual review alone.
Source:
- Nature Medicine AI Studies
https://www.nature.com - Google Health AI
https://health.google
Finding the Needle in the Haystack: How AI Analyzes Your Lab Results and Medical History
An additional benefit to improving health professionals’ abilities to analyze medical images is the “waiting” time after an X-ray, MRI, or CT scan. The process begins once a test is performed. A radiologist reviews the test results while you wait. In this role, the radiologist looks at the image(s) produced by the medical imaging device for signs of illness.
An example of an extremely knowledgeable and hypothetical “assistant” to the radiologist who assists them in analyzing test results and recalls countless previous tests is nearly identical to what we have today with Artificial Intelligence (A.I.) assisting health professionals in protecting them from missing potential issues.
How does it work? Large libraries of anonymous medical images are used as the basis for testing. The diagnosis is clearly identified; i.e., thousands of mammography images taken either with or without indication of cancer. The AI learns to recognize small, detailed patterns indicative of various diseases by analyzing many different examples. The AI can spot a small lung tumor or a faint shadow on a chest X-ray that might be difficult for a single doctor to notice in a single view, particularly if they are tired late in their workday.
In addition to helping prevent diagnostic errors, the AI serves as a protective barrier. By continuously flagging potential issues to the doctor for further review, the technology aids in faster diagnoses and, in turn, better treatment options for patients. Many hospitals across the U.S. that use machine learning technology for medical diagnosis are finding that it gives doctors greater confidence in making decisions about patient priorities.
Important to note, the AI will not make any decisions. The primary job of the AI is to identify specific areas of interest in a scan that require further review by the human radiologist. Using the information provided by the AI, along with their extensive experience and medical knowledge, the radiologist makes all of the decisions.
Always retaining complete authority over your medical care, the doctor will use both the information found by the AI as well as their own expertise to determine whether a particular area of concern warrants further examination. While the AI’s ability to find the “needle in a haystack” in images is one piece of the puzzle, AI is now beginning to look at additional forms of complex data associated with each patient’s history, including lab results and prior medical histories.
From “One-Size-Fits-All” to “Made-For-You”: AI’s Role in Personalized Treatment Plans
Beginning with years of medical treatment based on what worked for the “average” patient and ending in a long cycle of trial and error, this era of one-size-fits-all medicine ultimately produced a medication that saved someone’s life but had virtually no effect on another.
However, we are entering a new age of medicine, utilizing artificial intelligence (AI) to develop personalized medicine. This will finally end the days of “a pill for everyone.” Custom-made suits are purchased differently from those bought off the rack. Similarly, by using a person’s unique biological data, AI can help physicians determine the best treatment for each individual.
Perhaps no area of medicine could benefit more from AI in developing targeted therapies for complex cancers such as lung cancer. Physicians currently utilize about 12 different medications to treat lung cancer. Ultimately, the choice of medication is usually made on generalized statistical evidence.
Using AI to create individualized treatment plans provides a more precise way to select the right treatment. AI analyzes the genetic makeup of a tumor and compares it to a large database of tumor profiles and their respective treatment successes and failures in order to identify which treatment will work best for the particular tumor type – also referred to as targeted therapy.
Overall, the process is quite easy and takes place over three basic steps:
- Health data is collected about you. This is all your genetic information, your entire medical history, and what you have done with your life (e.g., eating habits).
- AI Analysis of your data. Your health data is compared by the AI to literally thousands of similar patient’s data and their respective outcomes based upon the treatments they were administered.
- Your doctor receives a ranked list of potential treatment options. The top-listed treatment option(s) would be the most likely effective treatment option for you, while the bottom of the list would include the least likely to achieve a good outcome.
Much of this reflects the near future of artificial intelligence (AI) in medicine. Patients benefit greatly from this highly customized medical treatment because it increases the likelihood of a successful outcome earlier in the process, reduces debilitating side effects from unsuccessful treatments, and decreases the overall time spent on ineffective treatments.
However, customized medical treatment is not just used for managing serious diseases. The advancements in personalized medicine are also affecting how we manage our everyday lives and health, sometimes through technologies that can be carried in one’s hand.
Your Personal Health Guardian: How AI Works with Wearables and Apps
In a sense, there will be a new generation of “tailored” medical treatment. The earlier “large hospital” approach to “tailored” medical treatment can now be miniaturized and integrated into small, portable devices such as smart wearables and mobile phones.
Many of us have already begun using mobile applications to monitor our daily activities (such as how many steps we take each day) and sleep patterns, all using the same wearable smartwatches. Since the introduction of Artificial Intelligence (AI), many of our portable devices are becoming personal health management tools, especially for those with chronic diseases.
The technology takes the raw data collected through your device (i.e., how many steps you took yesterday) and converts it into useful, timely information. Raw data is converted into valuable, actionable alerts via the application of artificial intelligence. For instance, when you utilize a mobile app to track your heart rate, the app does not simply collect the data as a raw number. Instead, it determines what your average reading should look like, then reviews your readings against previous ones to identify any unusual patterns or trends that could suggest a potential issue.
The applications of these systems are vast; they allow people with chronic diseases (such as diabetes and/or heart disease) to have a great deal of control over their health. Moreover, by allowing patients to proactively monitor their health status in “real-time”, artificial intelligence (AI) can significantly enhance patient outcomes.
The above-described AI-based app, connected to a glucose monitor, would be able to determine whether there was a downward trend in the individual’s blood sugar levels and then prompt the patient to eat a snack before a possible serious health issue. In like fashion, it could send notifications to the patient, his/her family members/physicians regarding an abnormal heart rhythm that could be life-threatening.
While AI provides patients with the tools to make educated decisions relative to their own health, AI can also help physicians understand a patient’s health status better than ever before through the long term data collection.
Physicians are no longer forced to make informed treatment decisions based on just one snapshot of a patient’s health taken in the physician’s office. Through identifying trends within the collected data over weeks/months, physicians can now use that information to inform decision-making. Ultimately, physicians can utilize AI-based care for patients across the U.S., improving the quality of that care.
Although AI has enhanced our capacity to manage our health on a daily basis, another area where AI is helping to speed up the process of discovering new medical treatments is underway.
AI + Wearables Data Flow
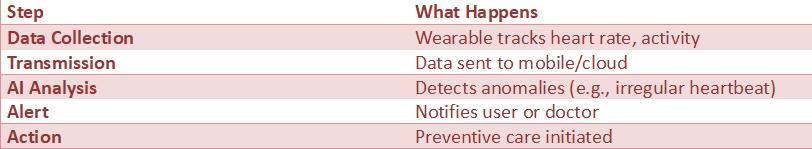
Example: Smartwatches can detect irregular heart rhythms and alert users early.
Source:
- Apple Health Research
https://www.apple.com/healthcare - Mayo Clinic Digital Health
https://www.mayoclinic.org
Speeding Up Cures: How AI is Helping Create New Medicines Faster
The development of drugs to combat diseases like Alzheimer’s, Cancer, or Rare Genetic Disorders is a long and frustrating endeavor. It has remained similar to the days of discovering new medicines, when finding a cure was much like searching for a “key” among billions of possible keys to unlock it.
Using the traditional “trial-and-error” method takes, on average, over a decade and costs Billions of dollars to create just one new drug. One of the most promising uses for Healthcare AI in the U.S. today is how quickly it can reduce the time spent looking for that key.
A researcher may spend years testing compounds in a laboratory setting, where AI can do the same “sifting through” portion of the search process in a matter of hours.
AI has the potential to help doctors find treatments faster because it can analyze vast amounts of data — both how drugs interact and what makes people sick — and identify candidates most likely to work, helping guide scientists toward a cure. Contrary to what many people believe, AI in drug discovery and development is meant to serve as a tool for doctors, not replace them. It’s intended to give doctors a better chance of narrowing down their options, ultimately saving time on research timelines — sometimes years’ worth.
There are two ways AI can be used effectively in medicine — the first is by developing entirely new medicines. The second is by discovering new uses for already approved medicines. Using this type of AI technology allows researchers to take thousands of currently approved medicines and discover surprising new uses for them.
For example, an AI discovered that a medication approved to treat high blood pressure also had properties that could slow the progression of neurodegenerative diseases. The future of artificial intelligence in medicine will provide us with a smarter, faster pathway to treatment, allowing life-saving cures to patients sooner than ever before.
The role of AI in laboratory settings is to assist in the search for cures. However, its involvement in more hands-on medical procedures may raise additional questions.
Is a Robot Performing My Surgery? Clarifying AI’s Role in the Operating Room
Robots and surgery seem like something straight out of a sci-fi movie, potentially leading to doctors being replaced and robots making life-or-death decisions. But there is a big difference. Robots do not make decisions, nor do they perform cuts on patients. What you get from robotic-assisted surgery is an extremely sophisticated toolset that enables a human doctor to make precise movements. Most robotic-assisted surgeries today integrate artificial intelligence (AI), combining human and machine.
For example, during a robotic-assisted surgery procedure using AI, the surgeon sits at a console next to the patient (usually just a few feet away), looks at a 3D HD monitor, and operates the robotic arms with hand controllers. Each time the surgeon moves, the robotic-assisted system converts that movement into an exact, tiny, consistent movement inside the patient’s body; all small hand motions caused by normal hand shaking are also eliminated.
The issue here is not about battling human physicians against AI physicians who can diagnose and give good care. It is really about giving a very skilled physician a clearer picture of what he/she is doing and a steadier hand so that the physician can complete a complex surgery with greater accuracy than would be possible without this technology.
There have been many tangible advantages for patients from robotic-assisted surgical technologies. These technologies allow surgeons to create significantly smaller incisions than would occur during traditional open surgeries. Smaller incision sizes generally mean less post-operative pain for the patient, smaller scars, and shorter recovery times. In addition to faster recoveries, these tools enable physicians to get patients back to their regular routine sooner than they would without these advances.
One might say this type of “hands-on” assistance is among the best ways AI has helped physicians with medical diagnosis and treatment. Nonetheless, there are many significant concerns associated with the use of this technology. Two of the most relevant concerns involve the data collected by these systems and how those systems may affect medical decision-making.
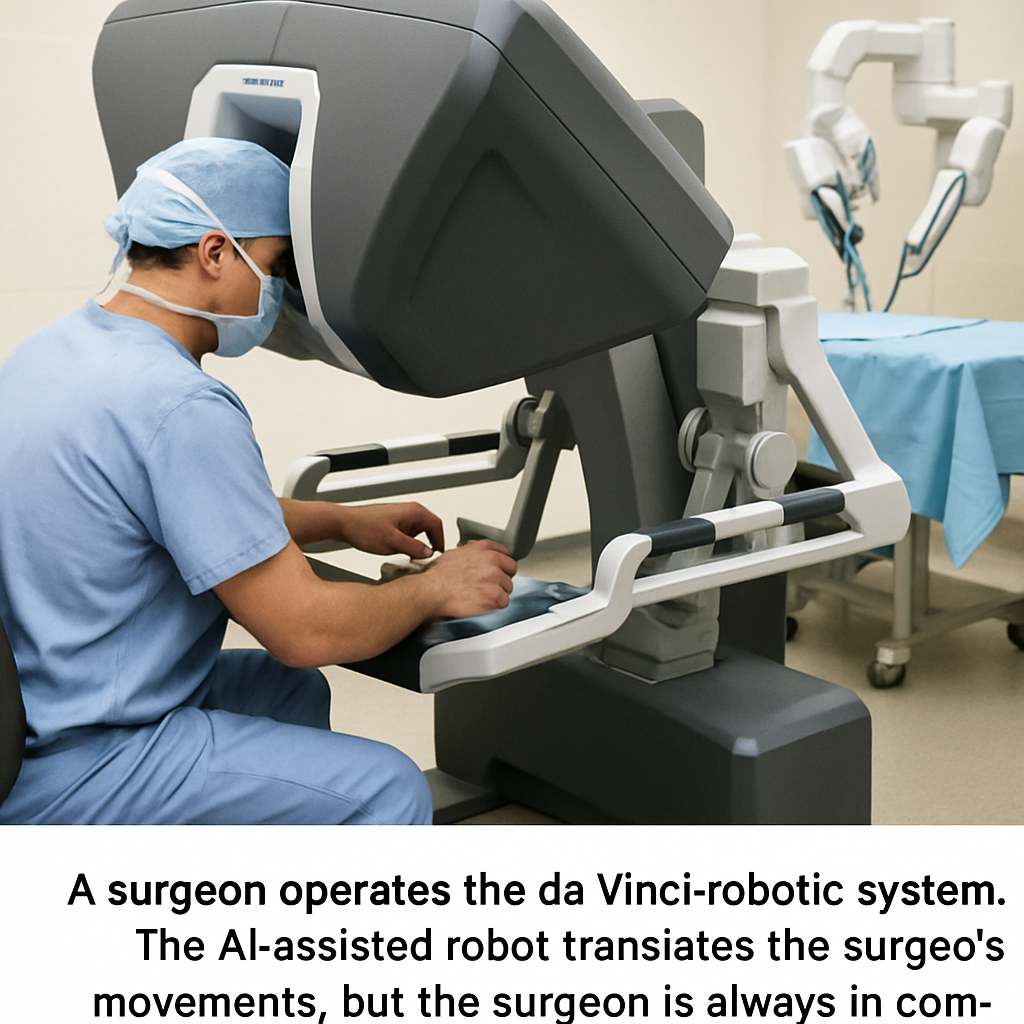
A surgeon operates the da Vinci robotic system. The AI-assisted robot translates the surgeon’s movements, but the surgeon is always in command.
Pros and Cons of AI is used in Healthcare in the USA: Examine the pros and cons of AI in healthcare to understand its benefits and challenges
There are many advantages to using Artificial Intelligence (AI) in U.S. healthcare systems, but there are also serious clinical, legal, and ethical implications to consider. Therefore, hospitals, clinicians, and patients should be aware of both the positive and negative implications of using AI responsibly.
Pros
- Early diagnosis and detection. AI can scan medical images from radiology studies, pathologic examination slides, EKGs, and laboratory tests to recognize patterns indicating conditions such as stroke, cancer, sepsis, or heart disease. The earlier an issue is identified, the sooner a physician can begin treating a patient and make an effective decision about admission.
- Efficiency increase and decrease in administrative burden. AI can generate physician orders, write clinical notes, compile summaries of the patient’s chart, help in coding, and support the prior authorization process. If used properly, these duties will allow clinicians to focus on other patient-care tasks and, hopefully, improve service availability by enabling them to treat more patients.
- Personalized Medicine. Predictive models will identify individuals at elevated risk of hospitalization due to complications or readmissions. This will empower the care team to proactively develop strategies to manage risks through outreach, remote monitoring, and the management of chronic conditions before they become severe issues.
- Improved Operational Performance. AI can forecast how many personnel will be needed to care for all patients, and will help determine the best schedules for each employee based on staffing needs. Additionally, AI can help streamline bed management and discharge planning, reducing bottlenecks that negatively impact the patient experience.
Cons
- Disparities in risk created by bias/inequality in training data: If the training data for an algorithm does not represent all demographic groups within a given population, then the algorithm will make inferior recommendations to that group, as well as increasing disparities in diagnostic assessments, pain evaluations, referral processes, etc., or risk score(s).
- Increased risks of privacy and security breaches: The United States has a high level of sensitivity surrounding health-related data (HIPAA compliant), and there is a higher likelihood of exposing this data through shared data, utilizing third-party vendor applications/models, especially in cases where patient communication/messaging or remote monitoring are used.
- Safety/Reliability Risks due to Black Boxes: Clinical workflow may be disrupted and/or the model may fail due to declines in data quality and/or changes in the patient population from those originally modeled against. In addition, the lack of explainability for alerts that have been triggered or failed to trigger creates uncertainty regarding decision-making.
- Inconsistent Regulatory/Liability Environment: There is an uneven regulatory environment for some technologies, as some fall under FDA regulation while others do not, creating inconsistencies. Further complicating the issue is determining liability when errors occur: because AI contributes to an error, it becomes unclear whether the clinician, hospital, vendor, or other stakeholders are liable.
- Poorly Implemented Systems Create Workflow Interruption/Anti-Trust Risks: Poorly developed systems result in “alert fatigue” among medical staff, creating distrust and further disrupting workflow.
U.S. adoption of AI-based technologies in healthcare must be balanced by appropriate validation of the technology, ongoing performance monitoring, testing for biases in training data, governance, and clear human oversight to ensure that the benefits of AI exceed the associated risks.
Pros and Cons of AI in Healthcare
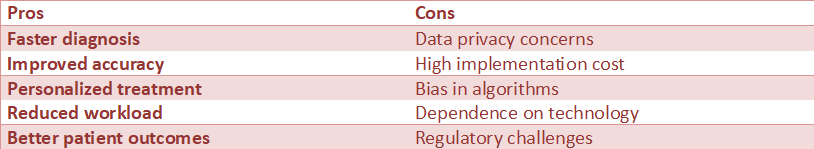
Key Insight: AI offers major benefits, but must be balanced with ethics, privacy, and oversight.
Source:
- World Health Organization (AI Ethics)
https://www.who.int - Harvard Medical School AI
https://hms.harvard.edu
The Big Questions: Is AI Safe and Is My Health Data Private?
Questions arise when you employ AI in healthcare, e.g., when using AI to analyze your medical history. Who can protect this sensitive medical information against improper use? And do we believe these “smart” systems will function equally effectively across all populations? For those developing and utilizing the systems, neither of these issues is secondary – they are primary issues being addressed.
Fortunately, there are numerous levels of security to protect your medical information. I am sure you have heard of HIPAA (Health Insurance Portability & Accountability Act), which provides a layer of confidentiality surrounding your medical records. Additionally, HIPAA applies to any Artificial Intelligence System that accesses or processes your patient data.
Therefore, if an entity uses an AI tool to process patient data, it must provide evidence of compliance with both HIPAA & AI standards. This means that the AI cannot access any more data than is necessary to perform its specific task. Additionally, your data is treated with the same level of confidentiality as all of your other medical data.
A new problem has arisen from the use of AI: algorithmic bias. The quality of an AI System is directly correlated with the quality of the training data it receives.
AI has already been shown to have problems when systems are trained only on images of lighter-skinned individuals. When these AIs are used to diagnose dark-skinned patients with skin cancers, they often fail. This is algorithmic bias in its most basic form. Bias within AI can create serious inequalities in access to quality medical treatment. While an AI system may be great at treating one demographic group, it is failing to treat others. There is no error in the technology itself; there is an error in providing quality care for everyone.
Recognizing the issue as a key focus, researchers and regulatory agencies are working to develop larger, more diverse training sets for AIs. Many researchers are also working to make their AI more equitable and fair by including people from diverse racial, ethnic, and demographic backgrounds. However, while researchers want to create a very powerful AI, they want to create a powerful AI that provides safe and effective care for every patient. As AI begins to become a part of your healthcare team, how you build them will determine if they are trustworthy members.
Your Partner in Health: What AI Really Means for Your Future Care
The increasing adoption of artificial intelligence (AI) by physicians and other healthcare providers has led many to wonder whether AI systems used to analyze their health data would properly protect their private health information and fairly apply the analysis to everyone. These are just two of the main concerns currently being researched and developed by both AI developers and physicians.
Fortunately, several methods have been established to protect your private health information. HIPAA (the Health Insurance Portability and Accountability Act) is a federal law that sets up a “firewall” around your private medical information, protecting it from unauthorized access or use. HIPAA also offers the same type of protection for AI systems that handle patient information.
To comply with HIPAA requirements for using an AI system to manage patient information, the system must meet all required HIPAA standards. For example, when receiving patient information, the AI system must provide methods to secure and anonymize it. Additionally, the AI system may use only the patient information it receives to improve the quality of care for the individual and may review only the specific information it requires to complete its designated task. Under the same confidentiality guidelines that govern all aspects of your medical information, an AI system may not simply access a patient’s entire file for no reason.
Fairness presents a problem distinct from patient privacy protection: algorithmic bias.
AI systems will perform at their best when trained on the highest-quality data. In other words, an AI system designed to aid in identifying possible cases of skin cancer would likely be less successful at identifying skin cancer in someone who has darker skin, due to being exposed to mostly lighter-skinned patients during its development/training phase. Algorithmic bias is perhaps the biggest ethical concern related to the application of AI in healthcare. An unfair AI system could exacerbate existing disparities in access to equitable healthcare.
If an AI system works well for some but not as well for others (e.g., those of a particular race/ethnicity/gender), then that represents a failure to provide equal treatment to all patients.
Identifying the possibility of this occurring is the first step toward preventing it. Much of today’s research and regulatory efforts focus on ensuring that AI is developed using very large, diverse datasets that reflect the full range of our population. As such, researchers and regulators are working to create AI capable of incorporating data about every racial, ethnic, and demographic group represented by the general population.
Ultimately, the aim is to create more powerful and fairer technologies. Additionally, while the ultimate goal is to develop technology capable of assisting with your care safely and effectively, the process of creating AI should be undertaken with great care and consideration so that we can ultimately create a new trusted ally to support you and your doctor.
Conclusion
AI is now part of everyday healthcare in the United States, helping to make care faster, safer, and more personalized in many different ways. In addition to helping people schedule appointments, document their physician’s care, and reduce operational costs to decrease hospital waiting times and the amount of time spent receiving care, AI is also being used to support clinicians through the process of creating personalized decision-making resources.
Healthcare professionals are using AI to identify subtle findings in imaging studies, look for patterns in historical medical records and laboratory results, and alert clinicians to potentially life-threatening conditions, such as sepsis, early in the disease course. Therefore, AI can enhance the professional abilities of healthcare providers by enabling them to focus on high-priority matters.
In addition to supporting clinicians, AI is changing how healthcare is practiced by enabling the abandonment of “one size fits all” treatment protocols. Healthcare professionals are using AI to develop customized care plans based on a patient’s unique characteristics (e.g., genetic information, prior experiences/outcomes, and current monitoring). Wearable devices and apps will extend this type of service into home and mobile environments and allow patients to use ongoing insights to transition from managing chronic diseases to proactively managing them.
At the research level, AI is accelerating the discovery of new potential drugs and identifying new uses for existing pharmaceuticals. The ultimate measure of success, however, will not be how advanced the technology is but rather whether users eventually come to trust it.
Creating long-term value with AI is used in healthcare in the USA requires that health organizations protect the personal identifiable information (PII) of consumers who are utilizing these technologies. Organizations should also test and validate AI in actual clinical environments. Additionally, organizations should continuously monitor AI usage to ensure there are no inherent biases in the AI algorithm that result in disparate outcomes across populations. Lastly, while AI can recommend courses of action, prioritize items, and send alerts, healthcare providers must remain responsible for the final decisions regarding patient care and communication.
The most significant benefit of using AI is used in healthcare in the USA is that it provides clinicians with better tools to improve the timeliness, efficiency, and humanity of the overall healthcare delivery system for all.
FAQs
1) How AI is used in healthcare in the USA today?
AI is used in healthcare in the USA for scheduling appointments, documenting medical records, providing diagnostic support (e.g., image analysis), generating early warning signals (e.g., sepsis risk), remote patient monitoring, and operational planning (e.g., beds, staffing, patient discharge).
2) Does AI replace doctors and nurses?
No. For the most part, AI provides clinicians with an additional tool; it flags potential problems, summarizes relevant clinical information, or suggests possible courses of action — but ultimately the decision rests with a licensed healthcare provider who remains responsible.
3) How does AI improve diagnosis?
AI can provide a second set of “eyes” to assist clinicians in reviewing radiology and pathology reports, identifying potential problem areas, and prioritizing high-risk patients. Additionally, AI may synthesize lab values, vital signs, and patient histories to identify specific trends associated with a patient’s deteriorating condition.
4) Is AI making healthcare more personalized?
Yes. AI may help tailor treatment to individual patient characteristics, including history, comorbidities, and potentially genetic predispositions. Additionally, AI may support personalized patient monitoring programs for chronic disease management via wearable devices and/or remote patient monitoring systems.
5) Is my health data private if AI is involved?
It Should Be. AI technology that handles patient data is subject to HIPAA and other applicable security standards in the United States. The expectation is that all healthcare organizations and vendors that utilize AI technology will limit access, protect patient data, and comply with regulations.
6) What are the biggest risks of AI in healthcare?
The primary risks associated with AI in healthcare include: (1) Biases in AI results due to lack of diverse or representative data sets, (2) Privacy and security issues associated with the storage and transmission of patient data, (3) Lack of transparency (“black box”) regarding the rationale behind AI recommended courses of action, (4) Model degradation or drift over time which can lead to inaccurate results, and (5) Alert fatigue resulting from excessive notifications from AI.
7) What questions should patients ask their provider about AI?
Ask yourself: (1) Is AI being used in my care? (2) What type of data is AI using to inform my care? (3) Have the validation studies been completed for patients similar to myself? (4) Who reviews and verifies AI-recommended treatment options? (5) How am I assured that my personal health information is protected? (6) What are the consequences of an incorrect recommendation provided by AI?